In many homes, health management usually involves more than one person working together. Family members and caregivers may need to stay aligned with treatment plans and daily routines. Without a shared system, communication can slowly break down, and important steps may be missed. Many people have started using care management apps because they can simplify coordination and may reduce daily confusion.
They can also improve visibility and help ensure routines are followed more consistently. As digital tools evolved, healthcare gradually moved toward connected systems like CareClinic. These platforms can turn scattered data into coordinated actions and improve overall care outcomes.
Over the years, we’ve developed a lot of care management solutions powered by clinical data interoperability frameworks and real-time health data orchestration systems. As we have this expertise, we’re sharing this blog to discuss the steps to develop a care management app like CareClinic.
Why Care Apps Like CareClinic Are Growing Fast?
According to Grand View Research, the global care management solutions market size was valued at USD 14.67 billion in 2024 and is projected to reach USD 33.26 billion by 2030, growing at a CAGR of 14.8% from 2025 to 2030. This aggressive trajectory signals a fundamental restructuring of healthcare capitalization, as value migrates from fragmented legacy systems to unified, data-driven platforms.
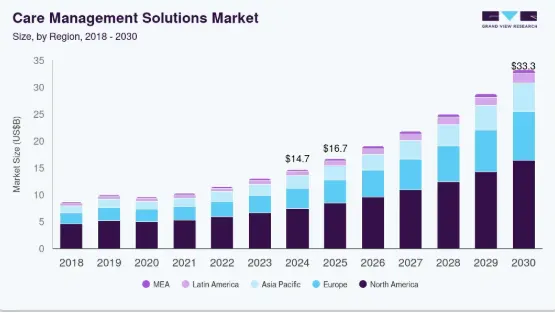
Source: Grand View Research
The ascent of platforms like CareClinic and ThoroughCare is fueled by a desperate need for decentralization as traditional healthcare hits an efficiency ceiling. By offering scalability that physical clinics lack, these apps capture high-fidelity longitudinal data that insurers and providers crave.
High-net-worth investors now recognize that owning the interface is the gateway to a proprietary data ecosystem that effectively controls the modern patient journey.
Rise Of Chronic Care Demand
Chronic disease management accounts for the majority of global healthcare spending. This fiscal pressure has turned Remote Patient Monitoring (RPM) into a requirement for modern health systems. Investors should note that demand has shifted from simple tracking to medical-grade monitoring of glucose, cardiac rhythms, and medication adherence in real time.
For a founder, the opportunity lies in the continuous data model. Unlike episodic care where a doctor sees a patient quarterly, care apps provide a 24/7 window into physiological states. Established players like HealthSnap and ChartSpan have already proven this by integrating RPM devices directly into clinical workflows, reducing emergency room visits and creating a clear ROI for payers.
Shift To Proactive Tracking
We are witnessing a pivot from sick care to well care. The legacy model is reactive, where patients seek help only after symptoms appear. This is the most expensive and least effective way to practice medicine. In contrast, care management platforms use predictive analytics to identify high-risk individuals before a clinical event occurs.
This shift is powered by AI-driven behavioral insights. By tracking micro-indicators like sleep changes or reduced activity, platforms like Lark Health and Omada Health can trigger proactive interventions. For an entrepreneur, this represents a transition from one-off consultations to a subscription-to-health model that insurance providers find highly valuable.
Gaps In Traditional Systems
Traditional healthcare suffers from a silo problem where patient data is trapped in incompatible systems. There is a lack of support in the 99% of a patient’s life spent outside the clinic. This gap is where billions of dollars in value are lost annually.
A care app fills this void by acting as a single source of truth. Platforms like Arcadia and Vim bridge the gap between specialists and patients by pulling data from fragmented records and making it actionable. Solving this fragmentation is a massive market opportunity for those building the connective tissue of the healthcare industry.
Market Signals For Founders
The most potent signal is the move toward value-based care reimbursement. Payers are shifting from paying for volume to paying for outcomes. This makes care management platforms an operational necessity for any medical group looking to remain profitable.
Additionally, the consumerization of healthcare is non-negotiable. Tech-savvy patients demand the same digital sophistication from healthcare as they do from banking, using tools like athenaOne or Epic’s MyChart to manage their own records. Investors must realize that the future belongs to the platforms that own the interface and the data rather than just physical real estate.

What Makes CareClinic A Benchmark Platform
CareClinic represents a sophisticated architecture that solves the app fatigue prevalent in digital health. While the market is flooded with point solutions, CareClinic functions as a comprehensive health operating system. It treats the patient as a whole entity rather than a collection of disconnected symptoms.
The platform value lies in its ability to centralize complex medical data into a single intuitive interface. By consolidating medication logic through the Dose Reminder and Symptom Tracker, it becomes an indispensable utility for high-value users managing chronic conditions.
Unified Care Ecosystems
The primary weakness of single-feature apps is data fragmentation. CareClinic eliminates this friction by creating a unified ecosystem. Once a user’s medical history and daily habit data are stored in the Health Diary, the switching costs become incredibly high, creating a critical moat for any founder.
Investor Insight: Value is proportional to data depth. A unified ecosystem captures longitudinal data that single-feature apps cannot access, creating a superior asset for valuation.
This approach allows for cross-variable analysis through Correlations and Insights reports. The platform can correlate medication dosages with sleep quality or blood pressure changes. For an investor, this translates to higher user retention and deeper data moats.
Care Team Collaboration
In traditional medicine, care teams rarely have access to the same information simultaneously. CareClinic solves this by enabling real-time data sharing through the Care Team feature.
- Continuous Feedback: Symptoms logged are immediately visible to authorized providers.
- Reduced Friction: Eliminates manual record transfers between different clinics.
- Active Intervention: Allows for treatment adjustments based on real-world data.
By utilizing the Care Plan module, stakeholders ensure every team member acts on the most current data available, differentiating a passive tool from an active clinical platform.
Data-Driven Insights
The future of healthcare investment lies in interpretation, not just collection. CareClinic uses algorithmic intelligence to surface trends, providing users with nudges and predictive warnings that move beyond legacy spreadsheet-style entry systems.
| Feature Component | Strategic Function | Investor Value |
| Vitals Tracking | Captures physiological data | High-fidelity clinical assets |
| Activity Logs | Monitors lifestyle factors | Comprehensive patient profiling |
| Proprietary Algorithms | Converts logs into Insights | Intellectual Property Moat |
By automating analysis through Vitals Tracking, the platform reduces the cognitive load on the patient. For an entrepreneur, the proprietary algorithm is the core asset that pharmaceutical companies and research institutions find most valuable for strategic partnerships.
All-In-One Retention
Retention is the holy grail of health tech. Users gravitate toward all-in-one platforms because they provide control over an overwhelming medical journey. When a platform manages everything from the Health Calendar to pill tracking, it transitions from a utility to a lifeline.
High engagement is driven by the platform’s ability to simplify life. By integrating Nutrition Tracking and Sleep Logs into one dashboard, all-in-one platforms build a level of trust that single-purpose apps cannot achieve. This long-term engagement is the foundation for a sustainable, high-margin business model.
Core Features Users Expect in Care Management Apps
Modern care management apps must transcend simple data entry to provide high-level utility for both patients and clinicians. For an investor, the value of these features lies in their ability to drive daily active usage while generating a robust, clean dataset.
A platform that fails to meet these baseline expectations will struggle to compete in an increasingly sophisticated market where users prioritize efficiency and data portability.
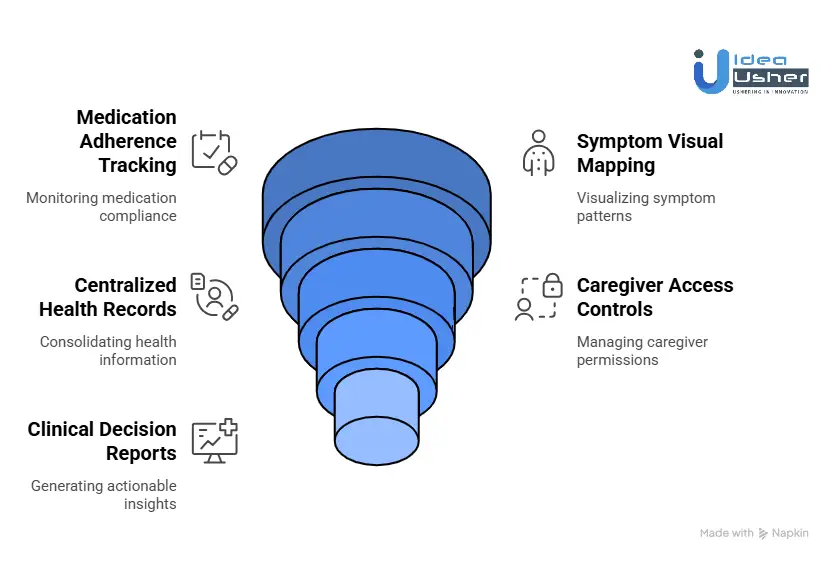
1. Medication Adherence Tracking
Sophisticated adherence tracking goes beyond basic notifications by incorporating complex dosing logic and drug interaction warnings. Platforms like Medisafe have set a high bar by providing granular compliance data that pharmaceutical companies and insurers find highly valuable for assessing treatment efficacy and long-term health outcomes.
2. Symptom Visual Mapping
High-value users require more than text-based logs; they need tools to map physical sensations to specific anatomical locations and intensities. Applications such as Bearable allow users to identify patterns between environmental factors and physiological responses, turning subjective experiences into structured, quantifiable data for clinical research.
3. Centralized Health Records
The modern patient often manages a fragmented history spread across multiple providers and portals. A centralized record system, a feature pioneered by platforms like PicnicHealth, acts as a digital vault for lab results, imaging, and vaccination records. This consolidation eliminates the silo problem and positions the platform as the user’s primary health interface.
4. Caregiver Access Controls
Healthcare is rarely a solitary journey, particularly for the elderly or those with chronic conditions. Robust access controls, seen in tools like CaringBridge, allow users to grant specific permissions to family members or professional caregivers. This feature expands the user base and increases platform stickiness across the entire support network.
5. Clinical Decision Reports
The ultimate goal of any care app is to facilitate better medical outcomes through data formatted for rapid clinical review. Instead of overwhelming doctors with raw logs, platforms like Propeller Health generate high-level summary reports that highlight trends and anomalies. These insights allow for more efficient consultations and data-driven adjustments to treatment plans.
Advanced Features That Drive User Retention
Retention in care management apps is no longer driven by simple utility but by deep, personalized value.
The most valuable platforms are those that move from being a digital notebook to an active intelligence layer. By leveraging advanced data processing, these apps transform raw data into life-changing behavioral insights that secure a permanent place in a user’s daily routine.
1. Correlation Engines
A true benchmark platform uses a correlation engine to identify hidden triggers that the human eye might miss. By analyzing relationships between medication schedules and symptom flare-ups, apps like Bearable help users understand the “why” behind health fluctuations. This feature provides immediate “aha” moments that secure long-term user loyalty.
Technical Moat: A correlation engine transforms a database into a diagnostic support tool. This shift from storage to analysis is what attracts institutional partners seeking real-world evidence.
2. AI Personalized Care
AI has shifted care plans from static documents to dynamic, evolving protocols. Modern platforms analyze user behavior to suggest adjustments to nutrition or activity levels. For instance, Lark Health uses AI to provide real-time coaching, making the experience feel bespoke.
- Dynamic Adjustments: Protocols update based on real-time biometric feedback.
- Behavioral Nudges: AI identifies the optimal time to prompt user engagement.
- Scalability: Automated coaching serves millions without increasing clinical overhead.
3. Wearable Integration
| Device Type | Data Stream | Strategic Utility |
| Smartwatches | Heart Rate / SpO2 | Continuous physiological monitoring |
| Oura / Whoop | Sleep / Recovery | Autonomic nervous system tracking |
| CGMs | Glucose Levels | Metabolic health and dietary analysis |
Integrating real-time vitals is now a baseline requirement for high-retention apps. By pulling data from various wearables, platforms like HealthSnap create a comprehensive profile. This seamless data flow reduces manual entry friction, keeping the app at the center of the user’s digital health ecosystem.
4. Mental Health Tools
Holistic care management necessitates the integration of mental health journaling and CBT modules. Providing structured prompts allows users to see the link between physical health and emotional well-being. This multifaceted approach, seen in platforms like CuraLife, increases daily active usage by addressing the user’s total health.
5. Predictive Risk Alerts
The transition from reactive to proactive care is anchored in predictive alerts. Using historical data, a platform can notify a care team when vitals trend toward a potential health risk. This early warning system is a massive value-add for insurers, as it demonstrably prevents expensive acute care episodes and hospitalizations.

How to Design UX for Long-Term Engagement?
Designing care management apps requires a delicate balance between medical utility and effortless interaction. If an interface feels like a chore, users will abandon it during their most critical recovery phases. The goal is to build a digital environment that feels supportive rather than demanding, ensuring the platform stays integrated into the user’s lifestyle over months and years.
1. Reducing Daily Logging Load
The friction of manual data entry is the primary killer of health apps. Successful platforms minimize this by using predictive text, one-tap logging, and smart defaults based on previous entries.
- Smart Defaults: The app remembers common dosages or meal times.
- Voice to Text: Allows hands-free logging for users on the move.
- Biometric Sync: Automates vitals to remove manual entry entirely.
By lowering the barrier to entry, apps like Mango Health ensure that even on bad days, the user can maintain their health record with minimal effort.
2. Designing For Multiple User Types
A care app is rarely used in a vacuum; it must cater to a care circle. This means the UX must shift seamlessly between a patient-facing dashboard and a caregiver-facing oversight tool.
UX Principle: The patient needs motivation and simplicity, while the caregiver needs high-level alerts and coordination tools. Apps like Zocdoc or CareZone succeed by creating specific views that serve these distinct psychological needs without cluttering the primary interface.
Neurodiverse User Accessibility
Accessibility is not a feature; it is a fundamental requirement. For neurodiverse users such as those with ADHD, autism, or cognitive impairment, the UI must be exceptionally clear. This involves using high contrast elements, avoiding sensory overload, and providing breadcrumb navigation to prevent confusion during multi-step processes.
| Design Element | Benefit for Neurodiversity |
| Consistent Iconography | Reduces the need to re learn the interface |
| Scheduled Reminders | Supports executive function and memory |
| Minimalist Layouts | Prevents overstimulation and decision fatigue |
Gamification Vs Clinical Seriousness
There is a fine line between making health fun and maintaining the gravity of medical management. While progress bars and streaks can motivate habit formation, the tone must remain respectful.
Platforms like SuperBetter use game mechanics to build resilience, but they avoid childish aesthetics that might undermine a doctor’s confidence in the data. The balance is struck by using gamification for behavioral goals like walking or drinking water while keeping clinical goals like heart medication strictly professional and direct.
Building HIPAA-Compliant App Architecture in Care Apps
Security is the bedrock of care management apps as data breaches in healthcare carry high fiscal and human costs. Building a HIPAA-compliant architecture is a core competitive advantage for any founder. A robust security framework ensures patient trust remains intact while allowing for the seamless exchange of medical information.
1. Encryption And Secure Storage
Data must be protected both at rest and in transit using industry-standard protocols. This involves encrypting databases and using secure tunnels for any information moving between the app and the server. Databases use AES 256-bit encryption to ensure data is unreadable if hardware is compromised.
- At Rest: Data is encrypted at the storage level.
- In Transit: TLS 1.2 or higher protects data moving across networks.
- Key Management: Encryption keys are stored in separate hardware modules.
By utilizing cloud providers like Aptible, developers can automate much of this infrastructure to maintain high security standards without slowing down the development cycle.
2. Role-Based Access Design
Not every user of a platform requires access to every data point. Role-based access control ensures that a physical therapist sees only what is relevant to mobility while a primary physician sees the full clinical history.
Privacy Principle: Access follows the rule of least privilege. This minimizes the risk of account compromise and ensures sensitive patient data is only viewed by those with a specific clinical need.
3. Audit Trails And Logging
Compliance requires a permanent and unalterable record of who accessed what data and when. Audit trails act as a black box for the application to provide transparency during a security review or a clinical dispute.
These logs track system entry through User IDs and timestamps while recording every modification to a health record. Monitoring data exports ensures that information leaving the platform is always authorized. This level of oversight is essential for maintaining the integrity of the patient journey.
4. Common Security Mistakes
Many platforms fail due to simple procedural oversights rather than a lack of encryption. One common error is failing to sign Business Associate Agreements with third-party service providers like email or analytics tools.
Another frequent mistake is the use of soft deletions, where data is hidden from the user but remains searchable in the database. Truly compliant platforms like TrueVault emphasize the importance of rigorous data lifecycle management to prevent the accidental exposure of legacy patient information.
How to Build a Care Management App Like CareClinic
Building a care management app like CareClinic usually starts with structuring patient data flows and defining how care plans will be tracked and updated in real time. The system should gradually integrate interoperability layers and may enable secure syncing so caregivers and providers can consistently access and act on shared health data.
Over the years, we have built multiple care management apps like CareClinic, and this is how we typically develop them.
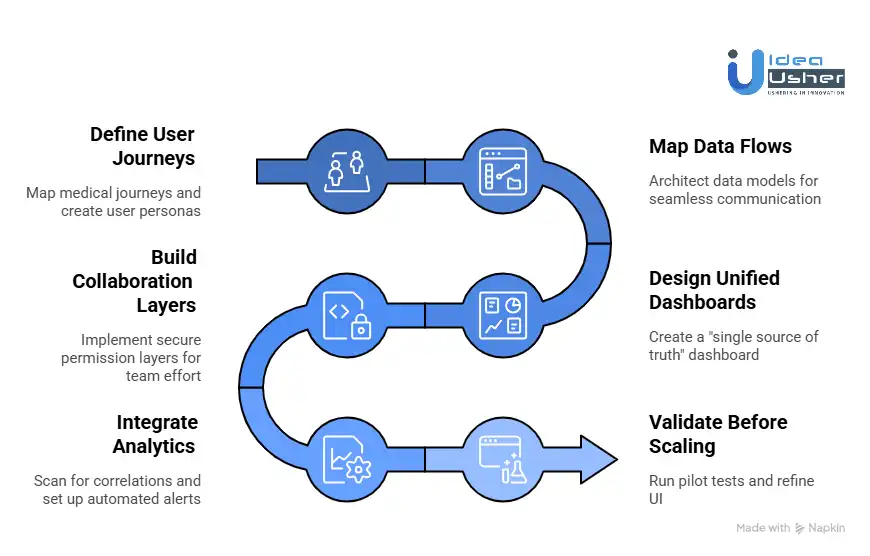
1. Define User Journeys
We map the specific medical journey your app will support, from chronic disease management to post-surgical recovery. Our team identifies the unique pain points of patients, doctors, and family members to create detailed user personas. This foundational step ensures every feature serves a clear clinical purpose and solves a real-world friction point.
2. Map Data Flows
A benchmark platform must handle fragmented data with precision. We architect sophisticated data models that allow symptom logs, medication schedules, and lab records to communicate. By structuring these data flows early, we ensure that a change in medication dosage can be cross-referenced with symptom intensity, creating a rich longitudinal record.
3. Design Unified Dashboards
We move away from cluttered interfaces by designing a “single source of truth” dashboard. Our UX team prioritizes high-level snapshots that highlight trends over raw data lists. This approach allows users to quickly understand their health status at a glance, reducing cognitive load while providing the insights that keep patients engaged.
4. Build Collaboration Layers
Healthcare is a team effort, so we build secure permission layers that allow patients to invite caregivers or clinicians into their circle. We implement real-time sharing features that ensure everyone is looking at the same data. This collaboration layer reduces communication gaps and allows for faster clinical interventions when a patient’s status changes.
5. Integrate Analytics
The value of the platform lies in its intelligence. We integrate custom analytics engines that scan for correlations between lifestyle factors and health outcomes. By setting up automated alerts for specific biometric triggers, we transform the app from a passive diary into an active monitoring tool that predicts risks.
6. Validate Before Scaling
Before a full-scale launch, we run rigorous pilot tests with actual patient groups to gather qualitative feedback. We analyze how users interact with core features and refine the UI based on real-world behavior. This validation phase ensures the product is technically sound, clinically relevant, and ready for high-volume scaling.

Cost to Build a Care Management App Like CareClinic
Building a care management app with the complexity of CareClinic requires a strategic financial roadmap. Because healthcare apps handle Protected Health Information, the “hidden” costs of compliance and security often outweigh the initial interface development.
When we estimate these projects for our clients, we categorize costs into distinct phases to ensure transparency and scalability.
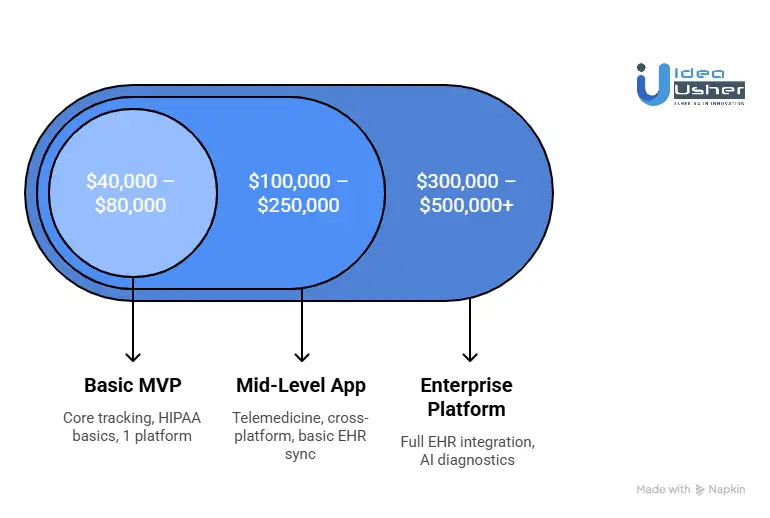
MVP vs Full-Scale Product Cost
A MVP typically focuses on the “Big Three”: medication tracking, symptom logging, and basic reporting. This allows you to enter the market quickly and gather user data. A full-scale product, however, includes advanced AI analytics, deep integrations, and multi-user collaboration layers.
| Product Stage | Estimated Cost (USD) | Timeline | Core Focus |
| Basic MVP | $40,000 – $80,000 | 3–4 Months | Core tracking, HIPAA basics, 1 platform |
| Mid-Level App | $100,000 – $250,000 | 6–9 Months | Telemedicine, cross-platform, basic EHR sync |
| Enterprise Platform | $300,000 – $500,000+ | 10+ Months | AI diagnostics, full EHR integration, predictive alerts |
Factors That Increase Development Costs
The “complexity tax” in healthcare is real. Beyond the number of screens, the primary cost drivers are the backend architecture and the level of regulatory rigor required.
- Compliance Depth: Implementing HIPAA is not a one-time task. It requires encrypted databases, automated audit logs, and session management, which can add 20% to 30% to the total budget.
- Platform Choice: Developing natively for both iOS and Android provides the best performance but doubles the frontend work. Many of our clients opt for cross-platform frameworks like Flutter to save approximately 30% on initial costs.
- UI/UX Sophistication: Designing for patients with chronic pain or cognitive fatigue requires extensive accessibility testing, which demands more senior design hours.
Third-Party Integrations Pricing Impact
Most modern care apps do not build every feature from scratch. Instead, they rely on a web of specialized APIs. While this speeds up development, it introduces recurring monthly “shelf-ware” costs.
Pro Tip: Integration is rarely a “plug-and-play” experience in healthcare. Connecting to legacy EHR systems via HL7 or FHIR standards requires specialized middleware and significant developer time for data mapping.
Common integration costs include:
- Video/Chat (e.g., Twilio, Zoom): $300 – $2,000 per month.
- EHR/EMR Access (e.g., Redox, Particle Health): $500 – $5,000 per month.
- Wearable Data (e.g., Terra, Terra): Volume-based pricing, often starting at $200 per month.
Maintenance and Scaling Expenses
Launch day is only the beginning of the financial journey. We advise our clients to budget 15% to 20% of the initial development cost annually for ongoing maintenance. This fund covers mandatory OS updates, security patches to combat new threats, and server scaling as your user base grows from hundreds to thousands.
Neglecting this phase is the most common reason health apps fail. Without “adaptive maintenance,” an app can become buggy or non-compliant within a single year of its release.
Why Fragmented Health Data Kills User Progress?
The modern patient journey is often a digital maze. When data lives in isolated pockets such as a heart rate on a watch, a prescription in a pharmacy portal, and symptoms in a paper diary, the user loses the big picture. For care management apps, solving this fragmentation is the key to preventing clinical stagnation and missed opportunities for recovery.
1. Data Silos Across Apps and Providers
Most patients today manage a fragmented ecosystem of health tools. One app tracks calories, another monitors sleep, and a third holds lab results. Because these systems rarely speak to each other, the patient is forced to act as a manual data broker.
Platforms like MyLinks attempt to bridge this gap by aggregating patient records, yet many users still struggle with data that doesn’t sync in real time.
- The Provider Gap: Doctors often lack access to the daily lifestyle data captured by patient apps.
- The Technical Barrier: Legacy hospital systems frequently use proprietary formats that block easy data sharing.
- The Fatigue Factor: Users quit apps when they have to enter the same information into three different places.
2. Missed Insights
When data is disconnected, the most valuable health asset correlation is lost. Without a unified view, a patient might not realize that their Tuesday migraines are linked to Sunday’s medication change or Monday’s poor sleep.
This is why apps like Guava focus heavily on importing data from every possible source to find these hidden links.
The Cost of Blind Spots:
A fragmented view leads to redundant testing and delayed diagnoses. In the United States, it is estimated that the lack of data interoperability costs the healthcare system over $30 billion annually in administrative waste and inefficient care delivery.
3. How Unified Platforms Improve Outcomes
Unified platforms solve the silo problem by acting as a central intelligence hub. By consolidating every data point into one timeline, the app transforms from a simple logbook into a powerful diagnostic ally.
| Feature | Fragmented Approach | Unified Approach (CareClinic Style) |
| Medication | Manual reminders only | Automatic drug interaction checks |
| Symptom Mapping | Subjective memory-based logs | Data-driven correlation with vitals |
| Provider Visits | Verbal summaries of history | Instant PDF clinical report sharing |
| Adherence | Low due to app fatigue | High due to centralized convenience |
When a platform brings everything together, the cost of managing health drops while the value of the data skyrockets. Users stay engaged because they finally see the direct impact of their habits on their long-term wellness.
Building a Single Source of Truth for Care Data
Creating a single source of truth is the core technical challenge for care management apps. By centralizing medication, symptoms, and appointments, we transform scattered notes into a reliable clinical record. This unified approach empowers patients and medical teams with data they can actually trust.
1. Centralized Health Dashboards
A well-designed dashboard acts as a health command center. We prioritize daily checklists, vital trends, and medication doses on the home screen to keep users focused. Visual cues like color-coded rings help patients understand their adherence at a glance without digging through complex menus.
2. Syncing Stakeholder Records
Health data must be accessible to the entire care circle. we build sync layers that allow patients to share their dashboards with family and doctors in real time.
- Instant Updates: Caregivers receive notifications the moment a symptom is logged.
- Privacy Control: Users choose exactly which data points are visible to specific people.
- Two-Way Sync: Integration ensures lab results flow directly from providers into the app.
Platforms like CommonHealth demonstrate this value by helping users securely aggregate and share records across different hospital systems.
3. Eliminating Manual Errors
Manual entry is the primary source of medical data errors. We mitigate this by automating data collection from pharmacies and insurance claims to ensure medication names and dosages are always accurate.
Data Integrity: Automated syncing prevents dangerous drug interactions that occur when a patient forgets to log a new prescription manually.
Apps like PicnicHealth excel here by digitizing every paper and electronic record for the user. This removes the logging burden and ensures the health timeline is complete and free of confusing duplicate entries.

Real-Time Care Sync Improves Outcomes in Care Management Apps
Real-time synchronization is the pulse of effective care management apps. By ensuring that every member of a patient’s support network sees the same data at the same time, these platforms move from passive observation to active, life-saving intervention.
Shared visibility for Families and Doctors
- Instant Notifications: Caregivers receive immediate mobile alerts the moment a patient logs a high-risk symptom or misses a critical medication dose.
- Unified Health Feed: Families and physicians access a live, scrolling timeline of health events, removing the need for stressful “status update” phone calls.
- Informed Appointments: Doctors enter consultations already briefed on the patient’s week, allowing more time for treatment and less for manual data review.
- Peace of Mind: Remote monitoring through apps like CaringVillage allows long-distance family members to stay connected to a loved one’s daily wellness.
Reducing Delays in Treatment Adjustments
- Rapid Response: Real-time sync allows clinicians to adjust prescriptions or care protocols immediately after seeing a negative trend in biometric data.
- Minimized Wait Times: Patients no longer have to wait for their next physical appointment to report a side effect; the data is flagged for review as it happens.
- Dynamic Care Plans: Health goals can be updated on the fly by a provider, showing up instantly on the user’s dashboard to guide their next action.
- Early Intervention: Platforms like FollowMyHealth enable proactive outreach, catching minor health fluctuations before they escalate into emergency room visits.
Preventing Miscommunication in Care Plans
- Version Control: Real-time updates ensure that everyone is looking at the most current medication list, preventing the use of outdated or discontinued scripts.
- Direct Messaging Layers: Integrated secure chat allows patients to clarify instructions with their care team instantly, reducing the risk of self-treatment errors.
- Audit Trails: A synchronized log creates an unalterable record of who gave what instruction and when, providing a clear history of the care journey.
- Language and Context: Visual dashboards help bridge communication gaps for users who may struggle to explain complex physiological changes verbally.
Why Insight-Led Care Apps Outperform Tracking Apps?
The era of passive monitoring is ending. While basic health trackers act as simple digital filing cabinets, the next generation of care management apps functions as an active intelligence layer. Users are moving away from platforms that simply ask “What happened?” and toward those that answer “What should I do next?”
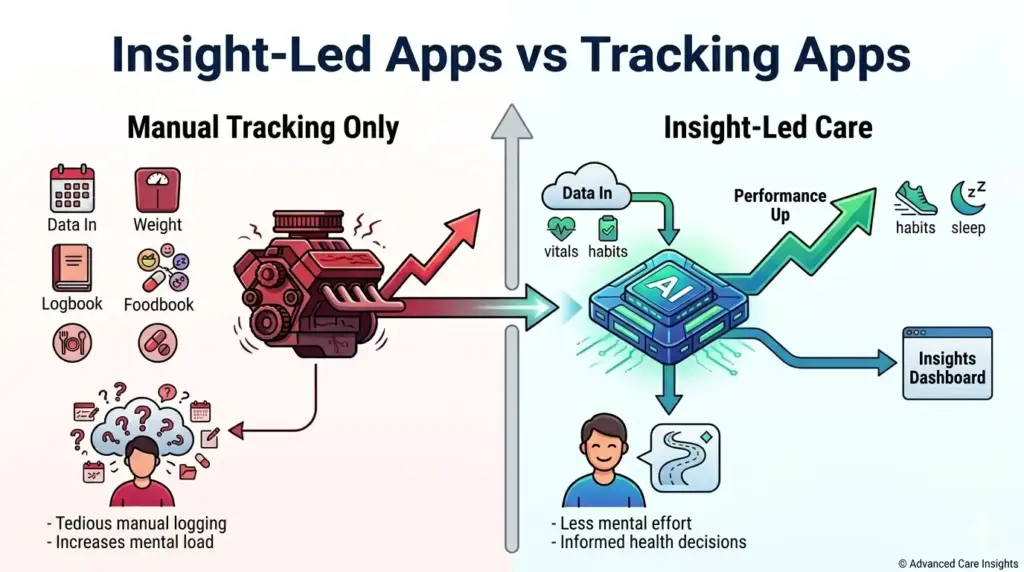
Modern healthcare technology succeeds when it reduces the mental burden on the patient. By shifting the focus from data collection to data interpretation, these apps provide the high-level clarity required for long-term health management.
1. Users Want Clarity, Not Just Data
A list of 50 blood pressure readings is just noise; a notification stating that “Your blood pressure spikes 20% every Tuesday morning” is a revelation. Insight-led design transforms abstract numbers into a narrative that patients can actually understand and act upon.
Apps like Wellthy lean into this by coordinating care tasks based on specific life events rather than just letting data sit stagnant.
The Cognitive Gap: Constant tracking without feedback leads to “data fatigue.” When a user does not see a correlation between their efforts and their results, they stop logging. Clarity re-ignites engagement by proving the utility of the habit.
2. The Shift Toward Recommendation Engines
We are seeing a fundamental transition from record-keeping to proactive coaching. Advanced platforms now use recommendation engines to suggest behavioral changes based on historical patterns.
- Contextual Nudges: Instead of a generic “Drink water” alert, the app suggests “Increase hydration today because your sleep quality was low last night.”
- Risk Prediction: Identifying trends that precede a flare-up, similar to how Ada Health uses probabilistic reasoning to guide users toward the right level of care.
- Dynamic Goal Setting: Automatically adjusting daily step or calorie targets based on the user’s current recovery phase or pain levels.
3. Designing For Decisions
The most effective UX designs are those that facilitate a specific choice. We move beyond “logging for the sake of logging” by creating interfaces that highlight “decisional triggers.”
This is exactly how Livongo became a leader in the space, by providing “health signals” that tell a diabetic exactly when to check their sugar or take a snack based on real-time trends.
| Feature Type | Tracking Focus (Old) | Decision Focus (New) |
| Medication | “Did you take it?” | “Is this dose causing your current fatigue?” |
| Activity | “How many steps?” | “Should you rest today based on your heart rate?” |
| Symptoms | “Rate your pain 1–10.” | “Your pain is rising; would you like to alert your doctor?” |
By framing the interface around choices, platforms help clinicians and patients make treatment decisions with higher confidence. This design philosophy ensures the platform is a partner in the care journey, not just a witness to it.
Why Choose IdeaUsher for Care Management Apps?
At IdeaUsher, we engineer high-performance care management apps built for real-world impact. With over 500,000 hours of coding experience, our team of ex-MAANG/FAANG developers brings elite technical precision to the healthcare space, ensuring every line of code is as reliable as a clinical prescription.
Proven Care Ecosystem Experience
We navigate the complexities of healthcare data, from pharmacy integrations to real-time vitals. Our team builds systems where fragmented data points communicate fluently, creating a single source of truth for patients and providers. We leverage pre-built healthcare modules to solve architectural hurdles before they become roadblocks.
Compliance-First Development
Security is baked into our lifecycle from day one. We implement a compliance-by-design framework that integrates HIPAA, GDPR, and HL7/FHIR standards into your app’s core. Our seasoned developers handle the rigors of encryption and audit trails without sacrificing speed, allowing you to focus on your clinical mission.
Scalable Go-to-Market Strategy
In digital health, speed is a strategic advantage. We use a modular, scalable architecture that allows you to launch a robust MVP quickly while leaving a clear path for future AI integration. By building for high capacity from the start, we ensure your platform remains stable as your patient base grows to an enterprise level.

Conclusion
Building a successful care management app requires balancing technical precision with deep human empathy. By focusing on a single source of truth and real-time data synchronization, you transform a simple tracking tool into a life-changing clinical partner. Partnering with a team that understands healthcare compliance and scalable architecture ensures your platform actively improves patient outcomes. The ultimate goal is to reduce the user’s burden while providing the clarity necessary for smarter health decisions.
FAQs
A1: Building a healthcare app starts with identifying a specific problem, such as chronic disease management or appointment scheduling, and conducting deep market research. You must then design an intuitive user interface, choose a secure tech stack, and ensure strict compliance with regulations like HIPAA or GDPR. The process typically concludes with developing an MVP, rigorous security testing, and post-launch maintenance to keep up with evolving medical standards.
A2: The 4 P’s of modern medicine represent a shift toward a proactive health model: Predictive, Preventive, Personalized, and Participatory. This framework focuses on using data to anticipate health issues, intervening before diseases develop, tailoring treatments to an individual’s unique genetic profile, and encouraging patients to be active partners in their own care.
A3: A HMIS is composed of five core pillars: Data Generation, Data Compilation, Data Analysis, Data Storage, and Information Use. These components work together to collect raw health facts, transmit them through the system, transform them into meaningful trends, and securely archive them so administrators can make informed decisions for hospital or national health planning.
A4: The primary difference lies in their scope and focus: an HMIS is an administrative tool used for managing hospital operations, finances, and overall health program planning. In contrast, an Electronic Health Record (EHR) is a clinical tool centered on the patient, designed to share comprehensive medical histories and real-time treatment data across different healthcare providers to ensure continuity of care.