Caregiving does not really switch off at night because uncertainty can quietly build with every small sound or movement. Many people have started using neurodivergent care apps because continuous monitoring can capture subtle behavioral patterns that manual tracking often misses.
The need for reliable alerts has also grown as safety concerns can arise without clear warning signs. These systems can convert observations into structured data, which is easier to analyze over time. Smart environments can also adjust lighting and sound to better support sensory regulation. This approach should make care more predictable without adding extra effort.
We’ve developed many neurodivergent care solutions that leverage technologies such as embedded IoT systems and behavior analytics frameworks. As IdeaUsher has years of experience, we’re sharing this blog to discuss the steps to develop a neurodivergent care app like Cubby Beds.
Why Smart Neurodivergent Care Apps Are in Demand?
According to Stratistics MRC, the Global Mental Health Apps for Neurodiverse Market is valued at $1.15 billion in 2025 and is projected to reach $3.66 billion by 2032, maintaining a 18.0% CAGR. This surge is driven by a critical shortage of clinical providers and a shift toward digital-first intervention. For investors, this represents a high-growth sector where early entrants are securing market share by prioritizing clinical validity over generic health tech.
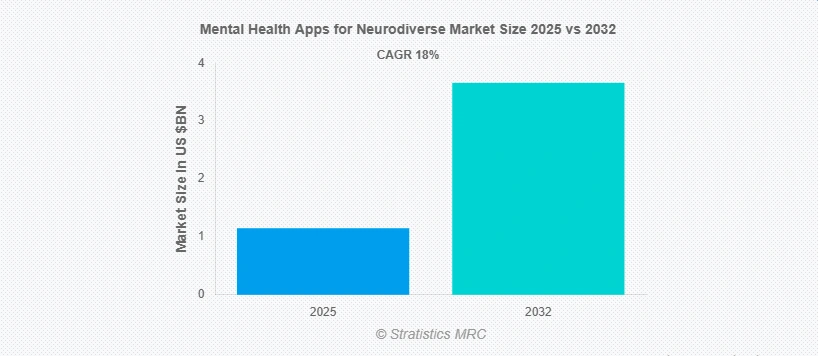
Source: Stratistics MRC
The market demand is fueled by the need for specialized ecosystems that address the complexities of ASD and ADHD. Beyond consumer sales, the Neurodiversity at Work movement has unlocked lucrative B2B enterprise contracts and insurance-backed B2B2C models.
These diversified revenue streams make the sector a primary target for capital looking to scale impactful, data-driven healthcare solutions.
Rising Need For Autism-Friendly Sleep Tech
Sleep disturbances are a central challenge for many neurodivergent individuals. Statistics show up to 80% of children with ASD experience chronic sleep issues. Traditional sleep apps often rely on blue-light interfaces or gamification, which are frequently overstimulating for this demographic.
There is a lucrative gap for low-arousal sleep technology. We are seeing a shift toward closed-loop systems that sync with smart home devices.
Platforms like Brain.fm have already demonstrated success by using patented, non-lyrical audio modulation specifically designed to support the ADHD brain in achieving sustained focus or sleep.
Gaps In Traditional Caregiving Solutions
The traditional caregiving model is fragmented and analog. Parents often juggle multiple point solutions for scheduling, therapy notes, and school coordination. This fragmentation leads to caregiver burnout and a lack of data continuity between different environments.
Modern platforms solve this by creating a centralized data repository. A valuable care app acts as an operating system where clinicians and parents observe real-time trends. For example, Tiimo has successfully addressed this by providing a visual daily planner that helps users manage transitions through a low-cognitive-load interface. Investors should prioritize platforms offering:
- Interoperability for pulling data from wearable devices.
- Secure, tiered access for different members of a care team.
- Active tools for visual scheduling and low-friction reminders.
Market Shift Toward Remote Monitoring Apps
We are witnessing a transition from static apps to dynamic remote monitoring systems. The value is no longer in providing a digital checklist but in the passive collection of data that predicts and prevents crises. These apps allow caregivers to monitor stress levels without being intrusive, fostering independence.
Strategic thinking in this space is moving toward Predictive Analytics. By monitoring heart rate variability or vocal patterns, an app can alert a parent before a sensory overload occurs. This transforms a utility app into a critical safety device, significantly increasing the lifetime value of the user.

Overview Of The Cubby Beds App
The Cubby Beds App is the digital core of an FDA-registered Class 1 medical device. It bridges the gap between physical safety and digital oversight for individuals with neurological challenges.
This interface is built for high-reliability monitoring rather than generic smart home use. It serves as the primary touchpoint for caregivers to interact with the bed’s hardware, creating a seamless loop of data through the Dream Hub. This integration ensures the app is a necessary component of the long-term care plan.
App–Hub Connection
The app connects to the physical Tech Hub (or the updated Dream Hub) via a secure, encrypted network. The Hub houses a 1080p HD camera, a microphone, and environmental sensors. Once synced, the hardware allows for immediate remote access via iOS or Android devices through the App Access feature.
This synergy is essential for safety. The app provides a Single Source of Control, ensuring only authorized caregivers can modify settings. By isolating controls to the app, the system prevents the occupant from accidentally disabling Safety Alerts or changing sensory inputs, maintaining a secure environment.
Core Modules
The app is architected into functional modules addressing specific neurodivergent care pain points:
- Remote Monitoring: Caregivers access a high-definition live feed with Night Vision and 4x Pinch-to-Zoom. It supports 24/7 Continuous Recording to help identify behavioral patterns or capture motion-triggered clips.
- Sensory Controls: This module manages Circadian Lighting and the Soothing Speaker for two-way audio or streaming pre-loaded nature sounds.
- Intelligent Safety Alerts: Using Motion + Sound Detection, the app sends real-time notifications. Sensitivity can be customized in the app to filter minor movements while flagging elopement attempts.
Caregiver Workflow
The app streamlines complex nocturnal routines. The workflow begins with the bedtime routine, where caregivers use the app to trigger calming sequences of light and sound. This reduces cognitive load and makes transitions more predictable for the individual.
During the night, the workflow shifts to passive monitoring. Caregivers use the 2-Way Audio and live feed to reassure the user remotely instead of risking a physical check-in. This data-driven approach replaces guesswork with actionable information, reducing chronic caregiver stress and improving the “Nighttime Enclosure” experience.
Key Benefits For Safety & Peace Of Mind
The primary ROI of the Cubby Beds App is the improved quality of life for the family unit. Research indicates these sensory-adapted beds can increase sleep duration from 4–6 hours to 8–10 hours per night. This measurable impact on health outcomes drives high retention and insurance eligibility.
Key benefits include:
- Reduced Elopement Risks: Digital fencing through Motion Alerts and Sound Detection prevents wandering.
- Enhanced Self-Regulation: Remote sensory adjustments via the Dream Hub allow for de-escalation without physical intervention.
- Caregiver Sustainability: Reliable 24/7 oversight through the Handheld Monitor and mobile app interface mitigates the burnout common in neurodivergent caregiving.
Key Features Users Expect in Neurodivergent Care Apps
Neurodivergent care apps focus on high-reliability monitoring and environmental control. Users expect military-grade security combined with a low-friction experience.
These platforms must prioritize fail-safe connectivity. A lag in a safety alert or a grainy feed is a critical failure in a care plan. High-value apps differentiate themselves by offering low-latency streaming to ensure the caregiver is never more than a second away from the individual’s needs.
1. Visual Oversight
High-definition oversight is the cornerstone of modern neuro-care. Users expect 1080p resolution with specialized night vision that avoids visible red lights, which can be overstimulating. Apps like Caniam provide high-quality video feeds, while features like pinch-to-zoom allow caregivers to monitor subtle cues like breathing patterns from a distance.
Investors should look for platforms offering 24/7 continuous recording with flagged motion-triggered events. This data is invaluable for clinicians assessing sleep hygiene or nocturnal behavioral patterns.
2. Vocal De-escalation
Two-way audio serves as a digital bridge for immediate reassurance. This allows caregivers to soothe a user without a physical presence that might otherwise escalate a meltdown. For example, AngelSense includes a “Listen-In” and two-way voice feature that lets parents talk to their child at any time without them needing to “pick up.”
For many, hearing a familiar voice through a high-quality speaker provides the grounding needed to return to sleep. This supports independence, allowing the individual to communicate needs without leaving their safe environment.
3. Intelligent Alerts
Reliable safety notifications are the primary driver of peace of mind. Users expect customizable motion and sound detection tuned to specific habits. SafeReturn is a specialized app that sends instant alerts if an individual prone to elopement leaves a safe zone, providing a “digital fence” for wandering.
The logic in these systems must be sophisticated enough to prevent alert fatigue. By filtering out normal sleep movements, the app ensures caregivers only receive notifications for significant safety events.
4. Light Regulation
Melatonin production is often disrupted in neurodivergent individuals, making automated lighting a critical feature. Users expect cycles that transition from energizing morning tones to warm amber hues. The Philips Hue app is frequently integrated into neuro-care routines to automate these transitions.
Remote control over light intensity allows for immediate environmental modification. If an individual wakes up disoriented, a soft, dim light can be triggered via the app to provide visibility without fully waking the user.
5. Auditory Control
Auditory processing issues make soundscape control essential. Neurocare apps must include a library of white noise and nature sounds to mask disruptive household noises. myNoise is a popular choice for this, offering calibrated soundscapes that can be shaped to specific frequency needs.
Advanced platforms integrate these into a bedtime routine. Caregivers can set timers that gradually taper volume as the user falls asleep. The ability to upload custom audio, such as a parent’s voice, adds significant emotional value.
6. Control Dashboard
A centralized dashboard serves as the command center for the entire system. Platforms like Mobile Caregiver+ provide a consolidated view of schedules and care tasks, while integrated smart-home dashboards allow for rapid atmosphere adjustments with a single tap.
For the investor, this builds long-term stickiness. By providing a single source of truth for safety and environment, the app transforms a smartphone into a monitor more powerful than any traditional camera system.
Advanced Features That Drive User Adoption
Next-gen neurodivergent care apps are moving from reactive alerts to proactive intervention. By integrating machine learning, these apps become active digital co-pilots. This technical shift is a key differentiator in the health-tech market. Strategic investors should prioritize platforms with clear roadmaps for the following capabilities.
1. AI Sleep Tracking
Modern platforms like SleepScore provide medical-grade analysis without uncomfortable wearables. These non-invasive systems use sonar or mattress sensors to track breathing and movement, identifying exactly where rest is disrupted.
For neurodivergent users, this uncovers “hidden” disturbances like sensory-triggered restlessness. The app correlates factors, like noise or temperature, with sleep quality, allowing caregivers to make data-backed adjustments.
2. Predictive Meltdown Alerts
Predicting emotional dysregulation is a high-value feature. Apps like Meltdown Monitor use algorithms to analyze real-time heart rate data for stress markers, triggering alerts minutes before a full meltdown occurs.
This allows for early de-escalation, such as automatically dimming lights to help the user self-regulate. For investors, this represents a significant technological moat requiring proprietary data and refined algorithms.
3. Custom Sensory Profiles
Because neurodivergence is a spectrum, leading apps like Inflow offer personalized profiles. Users can map specific sensitivities to light, sound frequencies, and haptic feedback.
These profiles ensure the app does not cause sensory overload. One profile might use high-contrast visuals for ADHD, while another prioritizes minimalist design for Autism, increasing long-term user retention.
4. Bedtime Automation
Automation reduces cognitive load for both users and caregivers. Apps like Tiimo allow for “Smart Workflows” that run on autopilot, gradually transitioning lights and activating white noise at set times.
These sequences provide the predictability essential for many neurodivergent individuals. By removing manual steps, the app reduces transition friction, making it a major selling point for busy families.
5. Wearable And IoT Integration
The future of neuro-care is an interconnected ecosystem. Strategic platforms are hardware-agnostic, pulling data from devices like the Apple Watch via hubs like Apple Health.
If a wearable detects a heart rate spike, the app can suggest a sensory break or adjust a smart thermostat. For investors, this interoperability is critical for scaling as new hardware emerges.

How Neurodivergent Care Apps Improve Safety and Sleep Quality?
The integration of smart technology into the bedroom does more than just monitor; it transforms the environment into a responsive sanctuary. For families utilizing neurodivergent care apps, where sleep is often a battleground of sensory input and safety risks, these digital tools act as an invisible, vigilant partner.
By centralizing control, caregivers can create a “closed-loop” system that anticipates needs and mitigates risks before they escalate into nocturnal crises.
1. Preventing Night Wandering
Wandering, or elopement, is a significant safety concern that often peaks during the quiet hours of the night. Traditional locks and physical barriers are often insufficient for a determined or disoriented individual.
Virtual Perimeters:
The app establishes a digital fence around the sleeping area. If the occupant crosses a predefined threshold, the system triggers an immediate, high-priority notification to the caregiver’s smartphone.
Instant Visual Verification:
Instead of rushing into the room and potentially causing more confusion, caregivers can instantly check a high-definition live stream to determine if the individual is simply repositioning or attempting to exit.
Predictive Motion Logic:
Advanced algorithms can distinguish between restless sleep and the specific motor patterns associated with “getting out of bed,” allowing for intervention at the earliest possible moment.
2. Reducing Sensory Overload
For many neurodivergent individuals, the world is too loud, too bright, and too unpredictable. Nighttime often amplifies these sensitivities, where a flickering streetlamp or a distant siren can trigger a full sensory meltdown.
Sensory Equilibrium: Through the app, the bedroom environment becomes a programmable bubble. Caregivers can automate the transition of light from stimulating blue tones to calming ambers, mimicking a natural sunset to trigger melatonin production.
Simultaneously, the app manages the “soundscape” of the room. By layering white noise or nature sounds, it masks disruptive household noises.
This level of environmental precision ensures that the brain isn’t constantly scanned for threats, allowing for a deeper, more restorative transition into REM sleep.
3. Improving Caregiver Peace Of Mind
The chronic stress of “sleeping with one eye open” is a reality for many families. The app significantly reduces this cognitive load by moving from manual oversight to automated vigilance.
| Traditional Monitoring | App-Integrated Monitoring |
| Frequent, intrusive physical room checks | Remote, non-intrusive digital check-ins |
| High risk of accidentally waking the occupant | Silent monitoring via smartphone |
| Constant anxiety over “silent” wandering | Guaranteed alerts for specific safety events |
| Guesswork regarding sleep quality | Data-driven insights into rest patterns |
This shift allows caregivers to achieve their own deep sleep, knowing that the system will only wake them if a genuine safety event occurs. This restored rest for the caregiver directly correlates to better patience, health, and quality of care during the waking hours.
How to Build a Neurodivergent Care App Like Cubby Beds?
A neurodivergent care app like Cubby Beds should begin with a secure data pipeline that connects sensors, cameras, and control systems into a reliable interface. It must carefully process motion sound and environmental signals to deliver real-time alerts while maintaining low latency and high accuracy.
We have developed multiple neurodivergent care apps like Cubby Beds, and this is how the approach is structured.
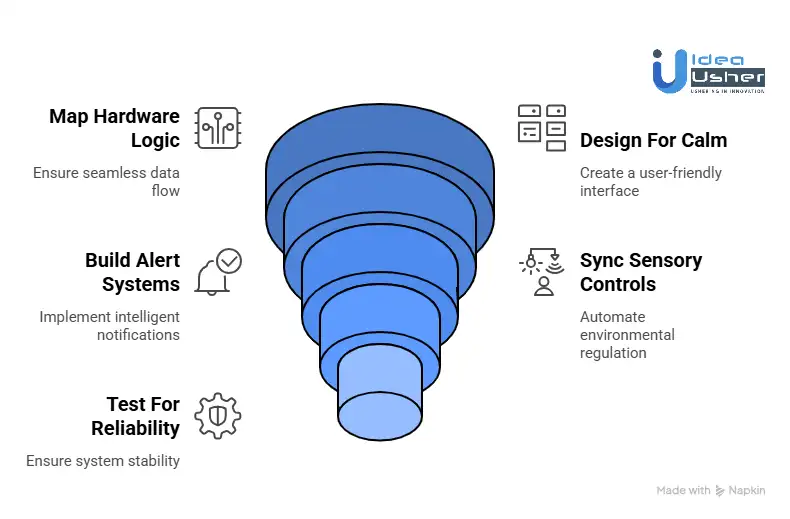
1. Identify Pain Points
We begin by immersing ourselves in the high-pressure reality of your daily caregiving. Our team identifies specific clinical risks, such as nocturnal wandering or sensory dysregulation, to ensure our roadmap solves your most urgent safety challenges. By focusing on these high-impact use cases, we build a foundation that directly mitigates caregiver burnout and provides a measurable return on safety.
2. Map Hardware Logic
A medical-grade app must act as the seamless brain of your hardware ecosystem. We map out the data journey from every sensor and 1080p camera to ensure information reaches your smartphone with zero perceptible lag. We specifically engineer the connection to be “fail-safe,” ensuring that critical alerts bypass silent modes and reach you even if the app is running in the background.
3. Design For Calm
We know you are often checking the app in low-light, high-stress conditions, so we design with a “calm-first” philosophy. Our UX team uses soft, muted color palettes and avoids aggressive animations or cluttered menus that could cause sensory overload. We prioritize large touch targets and intuitive navigation so you can make life-saving adjustments or view a live feed in seconds without a second thought.
4. Build Alert Systems
We develop a robust backend capable of processing live video and biometric data with military-grade precision. Our developers implement intelligent filtering that can distinguish between a user simply shifting in their sleep and an actual attempt to exit the safety enclosure. This “smart alerting” is specifically designed to prevent notification fatigue, ensuring that when your phone vibrates, it actually matters.
5. Sync Sensory Controls
Environmental regulation is a core part of our “digital bubble” strategy for your clients. We build automation modules that allow you to program gradual transitions for lighting to help regulate natural sleep hormones. By integrating a library of frequency-calibrated white noise directly into the app, we give you the power to mask disruptive household sounds and create a predictable, soothing atmosphere every single night.
6. Test For Reliability
Before we hand over the keys, our QA team subjects the platform to rigorous stress testing for every “black swan” scenario. We simulate power failures, Wi-Fi drops, and hardware disconnections to ensure the system remains stable and notifies you of any system-level issues immediately. We don’t just test for bugs; we test for the peace of mind you deserve in every possible real-world situation.

Cost to Build an App Like Cubby Bed
Investing in a neurodivergent care app involves a strategic financial commitment that scales with the level of protection you want to provide. Because these systems often handle sensitive biometric data and require real-time hardware synchronization, the budget reflects a need for medical-grade security and fail-safe architecture.
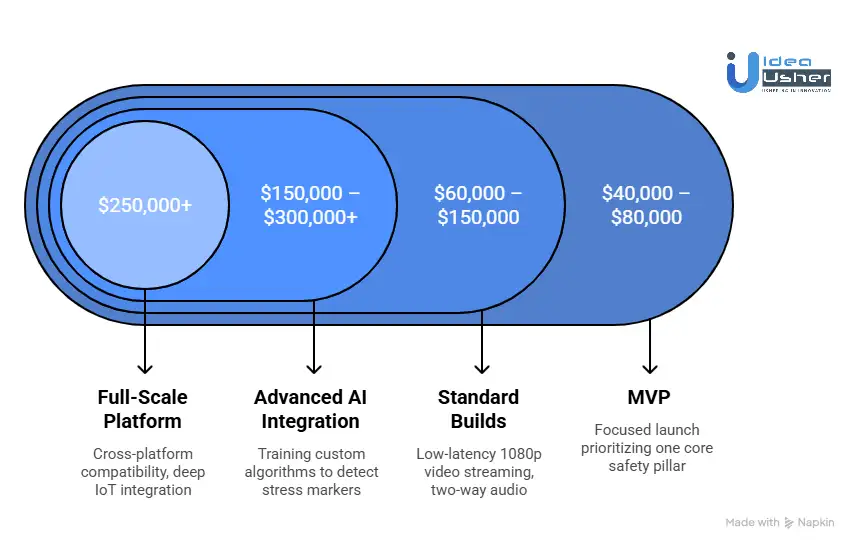
Cost Based on Feature Complexity
The price of development is primarily driven by how deeply the app interacts with the physical environment and the sophistication of its alert logic.
Standard Builds ($60,000 – $150,000): This covers the essential “digital bridge” between a caregiver and a user. It includes low-latency 1080p video streaming, two-way audio, and basic environmental controls for lighting and sound.
Advanced AI Integration ($150,000 – $300,000+): At this level, the cost increases as we implement predictive modeling. This includes training custom algorithms to detect “rumble stage” stress markers or distinguishing between normal sleep movements and an actual elopement attempt using machine learning.
MVP vs Full-Scale Platform Budget
Most founders begin with a Minimum Viable Product (MVP) to validate their specific care model before moving to an enterprise-grade solution.
Investment Tiers:
- MVP ($40,000 – $80,000): A focused launch that prioritizes one core safety pillar, such as high-definition monitoring and instant notifications on a single platform (iOS or Android).
- Full-Scale Platform ($250,000+): A comprehensive ecosystem featuring cross-platform compatibility, deep IoT integration for smart homes, and a clinical-grade dashboard for long-term behavioral data analysis.
Ongoing Maintenance and Upgrades
Building the app is only the first phase; maintaining a “never-fail” status requires consistent operational investment. Typically, you should budget 15% to 25% of your initial development cost annually to keep the system running at peak performance.
| Expense Category | Estimated Annual Cost | Purpose |
| Security Audits | $5,000 – $15,000 | Regular penetration testing and data compliance renewals. |
| Cloud Infrastructure | $6,000 – $24,000 | Hosting for encrypted video storage and real-time data processing. |
| OS & Device Updates | $4,000 – $10,000 | Ensuring the app remains compatible with new iOS/Android versions. |
| Feature Iterations | Variable | Refining the UI and alert logic based on caregiver feedback. |
What Makes Real-Time Safety Alerts Clinically Valuable?
In the field of neurocare, real-time alerts move beyond simple convenience and into the realm of clinical necessity. These systems act as a critical early warning layer, bridging the gap between passive observation and active medical intervention.
By leveraging high-sensitivity sensors, neurodivergent care apps can detect physiological and behavioral markers that are often invisible to the human eye, providing a data-driven safety net that traditional monitors simply cannot match.
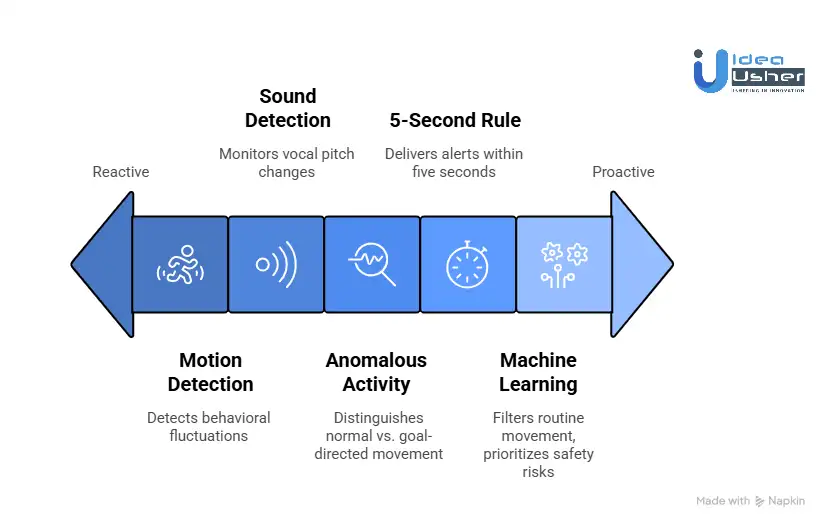
1. Motion And Sound Detection
Behavioral fluctuations during the night are often the first indicators of distress or a pending safety incident. Advanced apps utilize high-resolution telemetry to monitor for specific markers such as:
- Rhythmic Stereotypy: Identifying repetitive self-soothing or stimming motions that may signal rising anxiety levels.
- Vocal Pitch Analysis: Monitoring for changes in breathing or vocalizations that precede a meltdown or respiratory event.
- Anomalous Activity: Distinguishing between normal sleep cycle shifting and the goal-directed movements associated with elopement.
By capturing these ecologically valid markers in a home setting, the app provides clinicians with a clear window into the user’s moment-to-moment neurological state. This objective data reduces reliance on subjective caregiver reports, allowing for more accurate medication adjustments and behavioral therapies.
2. Faster Response Time
When a safety boundary is crossed, every second is a critical variable in the outcome. Research suggests that the most effective intervention is one that occurs at the rumble stage, the period immediately before a crisis peaks.
The 5-Second Rule:
High-reliability platforms are engineered to deliver emergency alerts within five seconds, breaking through do-not-disturb modes to ensure a caregiver is notified even during deep sleep.
This rapid notification allows for immediate vocal de-escalation via the app or a quick physical check-in before an individual reaches a dangerous exit or experiences a full sensory collapse.
The faster the response, the less likely the individual is to enter a state of high arousal trauma, leading to quicker recovery and better overall sleep quality for the entire household.
3. Trust Through Accuracy
The primary barrier to caregiver health is the chronic stress of alert fatigue, the psychological exhaustion caused by false alarms. Clinically valuable systems use machine learning to build a trust bridge by prioritizing significant events over routine movement.
| Reactive Monitoring | Proactive Trust Systems |
| Triggers for every minor movement | Intelligent filtering of normal sleep patterns |
| High rate of false alarms leading to muted phones | High confidence alerts for genuine safety risks |
| Caregivers remain in a state of hyper-vigilance | Caregivers can rest, trusting the system’s logic |
| Delayed or missed response to true crises | Immediate, priority delivery of critical notifications |
As the app demonstrates consistent accuracy, the caregiver’s baseline cortisol levels begin to drop.
This shift from hyper-vigilance to informed rest is a major clinical outcome, as improved caregiver sleep quality directly correlates to lower rates of depression, anxiety, and improved relationship quality with the care recipient.
Designing a Sensory-Aware UX for Neurodivergent Users
Designing for neurodiversity requires a shift from flashy interfaces to calm engineering. For many users of neurodivergent care apps, a standard interface’s bright colors or sudden animations are a source of genuine neurological distress.
Our design philosophy focuses on creating an environment that respects sensory boundaries while providing the caregiver with absolute clarity and control.
1. Simple UI For Focus
Visual noise is the primary enemy of focus for neurodivergent individuals. To combat this, we implement “Low-Arousal Design,” which prioritizes negative space and a restricted color palette.
For instance, Hiki uses a simplified interface to facilitate social connections for autistic users without the typical clutter of social media.
- Muted Tones: We avoid high-contrast white and neon colors, opting for soft ambers and deep indigos.
- Static Layouts: We remove auto-play videos and sliding carousels that can cause visual tracking issues.
- Predictable Navigation: Every icon is labeled clearly with text to reduce the cognitive load of interpreting abstract symbols.
2. Personalized Sensory Settings
Because neurodivergence is a spectrum, a one-size-fits-all interface is ineffective. We build deep customization suites that allow each individual to map their own sensory safe zone.
Apps like Otsimo exemplify this by offering highly adjustable settings for educational games, allowing parents to tailor the sensory intensity to their child’s specific needs.
Personalization Metrics: Users can adjust font weighting for dyslexia, toggle haptic feedback off for tactile sensitivity, and even shift the audio frequency of notifications to avoid “piercing” sounds that trigger a startle response.
This personalization ensures the app adapts to the human rather than forcing the human to adapt to the technology.
3. Control With Automation
The most effective care apps act as a quiet superpower that anticipates needs without stripping away user agency. We find the “sweet spot” by automating the environment while keeping the human in the loop.
For example, RoutineFactory helps automate daily tasks through visual aids while allowing users to check off accomplishments at their own pace.
| Automated Task | User Control Option | Clinical Benefit |
| Gradual Sunset Lighting | Manual Brightness Slider | Circadian rhythm regulation |
| White Noise Activation | Soundscape Library Selection | Auditory masking of house noise |
| Bedtime Sequence | “Snooze” or Delay Button | Maintaining a sense of autonomy |
This approach ensures the app provides the benefits of an intelligent assistant while maintaining the essential human checkpoints necessary for long-term trust and emotional safety.

How Circadian Lighting Impacts Sleep Onset in Cubby Bed–Like Apps?
For many individuals with neurological differences, the internal body clock doesn’t always sync with the outside world. This is where neurodivergent care apps step in, using environmental engineering to bridge the gap.
By manipulating the “color temperature” of a room, these apps can signal to the brain exactly when it is time to wind down and when it is time to wake up, significantly reducing the time it takes to reach sleep onset.
1. Digital Light Cycles
Our biology is wired to respond to the sun’s journey across the sky. In a clinical or home care setting, however, artificial “cool white” bulbs often disrupt this rhythm. Care apps solve this by automating a digital sky within the bedroom.
- Morning Blue Light: High-intensity cool tones to suppress lingering sleepiness.
- Midday Brightness: Full-spectrum light to maintain focus and alertness.
- Evening Amber: Warm, low-intensity light that mimics a setting sun.
By automating these transitions, the app removes the need for manual adjustments, ensuring the environment evolves naturally throughout the day without human intervention.
2. Melatonin Regulation
Melatonin is the “sleep hormone,” and its production is highly sensitive to light. Specifically, blue light wavelengths, common in tablets and standard LEDs, act as a chemical “off switch” for melatonin.
The Biological Mechanism:
When the app detects evening hours, it filters out blue light ($<450nm$) and shifts the room toward the red end of the spectrum. This chemical signaling encourages the pineal gland to begin melatonin secretion up to two hours earlier than it would under standard lighting.
This shift is particularly vital for those with ADHD or Autism, who may already experience delayed sleep phase syndrome. By “pre-loading” the body with its own natural sleep chemicals, the app helps bypass the typical bedtime resistance.
3. Lighting In Bedtime Routine
Predictability is a cornerstone of safety and comfort. When lighting is integrated into a multi-sensory routine, it acts as a non-verbal cue that the day is ending.
This automated “light story” provides a consistent, reliable structure. Instead of a sudden “lights out” which can be jarring or anxiety-inducing, neurodivergent care apps create a gentle, 30-minute fade that prepares the nervous system for rest long before the head hits the pillow.
- Preparation Stage: The system initiates a fade to 50% Amber, signaling a clear transition from high-energy play to a state of rest.
- Wind-Down Phase: Lighting shifts to a Deep Orange hue, specifically chosen to encourage physical relaxation and a quieter environment.
- Sleep Mode: The room moves into 1% Red or Total Darkness, allowing the user to maintain deep sleep cycles without the disruption of blue-spectrum light.
- Emergency Protocol: In the event of an alert, the app triggers an Instant 20% Warm White glow, providing safe visibility for the caregiver without causing sensory over-stimulation for the user.
Building a White Noise Engine for Sleep Stability
For many, the world never truly goes silent. In neurodivergent care apps, a white noise engine acts as an acoustic shield, masking unpredictable sound spikes that trigger startle responses. By creating a consistent auditory floor, the app helps the brain disengage from hyper-vigilance, allowing for a stable sleep cycle.
1. Calming Sounds for Sleep
The right soundscape is a calibrated frequency profile designed to soothe specific neurological patterns:
- White Noise: Equal intensity across all frequencies; ideal for masking sharp sounds like slamming doors.
- Pink Noise: Deeper waves, like steady rain; proven to improve deep sleep stability.
- Brown Noise: Bass-heavy, resembling a distant rumble; grounding for high sensory-seeking behaviors.
- Natural Textures: Organic loops of wind or fans that provide a non-repetitive backdrop.
2. Personalizing Audio Environments
Because every sensory threshold is unique, a one-size-fits-all track is insufficient. We build systems that allow for granular personalization of the “acoustic safe zone.”
The Sensory Palette: Caregivers can layer sounds, such as a Brown Noise base with a light fan texture, to create a custom frequency profile. Real-time EQ adjustments also allow the app to filter out specific high-pitched or low-end frequencies that the user finds distressing.
3. Continuous vs. Adaptive Playback
Stability is the goal, but delivery depends on the environment. We engineer two distinct modes to manage nocturnal challenges:
Continuous Playback:
This provides a constant, unchanging wall of sound throughout the night. It is the gold standard for individuals who require absolute predictability to maintain sleep.
Adaptive Sound Masking:
This mode is more reactive. The app uses the device’s microphone to monitor ambient room noise. If a sudden external sound is detected (like a dog barking), the app subtly and smoothly increases the white noise volume to “drown out” the intrusion before it wakes the user, then gently fades back to the baseline level once the environment is quiet again.
This intelligent modulation ensures the audio environment is always working to protect rest, whether through a steady state or reactive masking.
Why Caregiver-Controlled Apps Outperform Passive Devices?
Passive monitors often do little more than watch and wait. In contrast, neurodivergent care apps transform the caregiver from a passive observer into an active participant. By providing a direct interface to the user’s environment, these apps allow for immediate and nuanced adjustments that a basic “dumb” camera or a standard bed alarm simply cannot offer.
1. Real-Time Decisions
Data is only as good as the action it inspires. When a caregiver receives a notification, they should have the tools to intervene without even entering the room. This philosophy is seen in platforms like AngelSense, which provides continuous GPS and voice monitoring to allow caregivers to intervene the moment a boundary is crossed.
- Remote De-escalation: Use two-way audio to provide a familiar voice the moment a user wakes up.
- Environmental Triage: Instantly adjust the thermostat or lighting from the hallway to prevent a sensory meltdown.
- Contextual Alerts: Filter out false positives (like rolling over) so the caregiver only wakes up when a genuine safety boundary is crossed.
2. Higher Engagement
A high-quality care app does not feel like a chore; it feels like a natural extension of the caregiving routine. By simplifying complex data, these platforms keep caregivers engaged rather than burnt out.
For instance, Choiceworks helps manage daily routines and transitions through visual boards, making the management of care interactive rather than purely observational.
The Feedback Loop: Interactive dashboards allow caregivers to “tag” specific nights. If a user slept well after a specific white noise setting, the app logs that success. This creates a personalized user manual for that individual’s sleep health.
3. Measurable Outcomes
The ultimate goal of any neurodivergent care app is a tangible improvement in quality of life. Because these apps record every interaction and environmental change, they provide a level of clinical insight that passive devices lack.
Apps like Tiimo focus on executive function, providing a visual timeline that reduces the stress of “what comes next,” showing how active management leads to better daily outcomes.
| Metric | Passive Device Result | Controlled App Result |
| Sleep Onset | Unknown or Unchanged | Reduced by up to 30% via lighting |
| Meltdown Frequency | Recorded post event | Prevented via Rumble Stage alerts |
| Caregiver Stress | High constant checking | Lower trust in smart filtering |
| Data Accuracy | Anecdotal or Video only | Precise biometric and environmental logs |
This shift from watching to managing creates a safer and more predictable world. Caregivers gain the confidence to rest, knowing the app isn’t just a pair of eyes but an active guardian.
Future Trends in Neurodivergent Care Tech
Modern support for neurodiversity is evolving from reactive tools into proactive, intelligent ecosystems. As hardware becomes more discreet and software more human-centered, the next generation of neurodivergent care apps is shifting toward predictive care.
This transition ensures that support systems can anticipate needs and intervene effectively, staying one step ahead of a potential crisis.
1. AI-Driven Behavioral Insights
The move toward Agentic AI allows systems to analyze behavioral data and identify patterns invisible to the human eye. Apps like Brain In Hand already use digital tools to help users navigate high-anxiety moments before they escalate.
- Predictive Detection: Models track micro-fluctuations in vocal tone and motion to predict emotional overload.
- Interaction Tracking: AI monitors eye movement and facial engagement to provide real-time feedback on social comfort.
- Smart Summaries: Caregivers receive AI-generated highlights of meaningful changes in sleep or behavior.
2. Smart Environments and Automation
Care apps are becoming the brain for entire smart homes. This level of control is pioneered by platforms like LifeSkills, which use interactive prompts to help users master independent living.
The Adaptive Home: mmWave radar sensors detect a person’s presence and breathing rate even when they are still. This allows the app to maintain a “calm mode” while the user is present and automatically switch to “energy save” when they leave.
Local AI processing is also rising, ensuring sensitive data stays on a local device to increase privacy and speed for safety alerts.
3. Personalized Digital Therapeutics
Digital therapeutics (DTx) are evolving into regulated tools designed to improve cognitive functions. EndeavorOTC, for example, is a clinically validated video game treatment designed to improve attention in adults with ADHD.
Other emerging tools include:
- VR Exposure Therapy: Practicing social scenarios in a safe, controlled environment.
- Wearable EEG: Real-time focus tracking for improved executive function.
- Haptic Feedback: Gentle vibrations for task management and transitions.
- Social Robotics: Coaches that increase engagement and language skills in children.
By integrating these into a care app, the home becomes a site for continuous growth, empowering individuals to navigate the world with more independence.
Why Choose IdeaUsher for Neurodivergent Care Apps?
IdeaUsher can help you build cutting-edge solutions by leveraging over 500,000 hours of coding experience. Our team of ex-MAANG/FAANG developers understands the technical precision required to create empathetic, high-performance software for the neurodivergent community.
End-to-End Development Approach
We handle every phase of your project, from initial sensory-aware UI/UX design to final deployment. Our process ensures that features like circadian lighting and white noise engines are integrated seamlessly, creating a unified ecosystem that prioritizes the user’s neurological comfort.
Proven Track Record with Startups
Having launched numerous successful neurodivergent care apps, we know how to navigate the unique challenges of this niche market. We help startups move from concept to MVP quickly, ensuring your product is market-ready while maintaining the high ethical standards required for care-based technology.
Scalable and Secure Architecture
We build with the future in mind, using robust frameworks that grow alongside your user base. Our security protocols are designed to protect sensitive biometric and behavioral data, ensuring full compliance with global privacy standards while maintaining the speed needed for real-time safety alerts.

Conclusion
Building a neurodivergent care app like Cubby Beds requires fusing IoT environmental controls with empathetic software design. By centralizing circadian lighting, white noise, and safety monitoring into one interface, you create a digital “safe zone” that actively regulates sensory input. Success lies in balancing advanced automation with seamless caregiver overrides to ensure a predictable, restorative environment.
FAQs
A1: Successful development starts with inclusive, sensory-aware UX design that avoids overstimulation. You must integrate specialized features like circadian lighting, white noise engines, and routine builders using a robust IoT framework. The focus should be on building stable, low-latency systems that provide the predictability and safety these users require for daily functioning.
A2: These apps function as a centralized command center for a user’s environment and schedule. They connect to hardware via APIs to automate light and sound transitions while using sensors or manual inputs to track behavioral patterns. By analyzing this data, the app provides caregivers with actionable insights and allows them to adjust the environment in real-time to prevent sensory overload.
A3: The cost typically ranges from $40,000 to $150,000+, depending on complexity, platform requirements, and the level of IoT integration. Factors such as HIPAA compliance, AI-driven predictive analytics, and custom hardware syncing will influence the final budget. Starting with a Minimum Viable Product (MVP) allows you to test core features with users before scaling.
A4: Most platforms utilize a subscription-based model for families or a licensing fee for clinical care facilities. Additional revenue streams include one-time hardware sales, premium features such as advanced AI behavioral reports, or partnerships with insurance providers who may cover the app as a digital therapeutic tool.